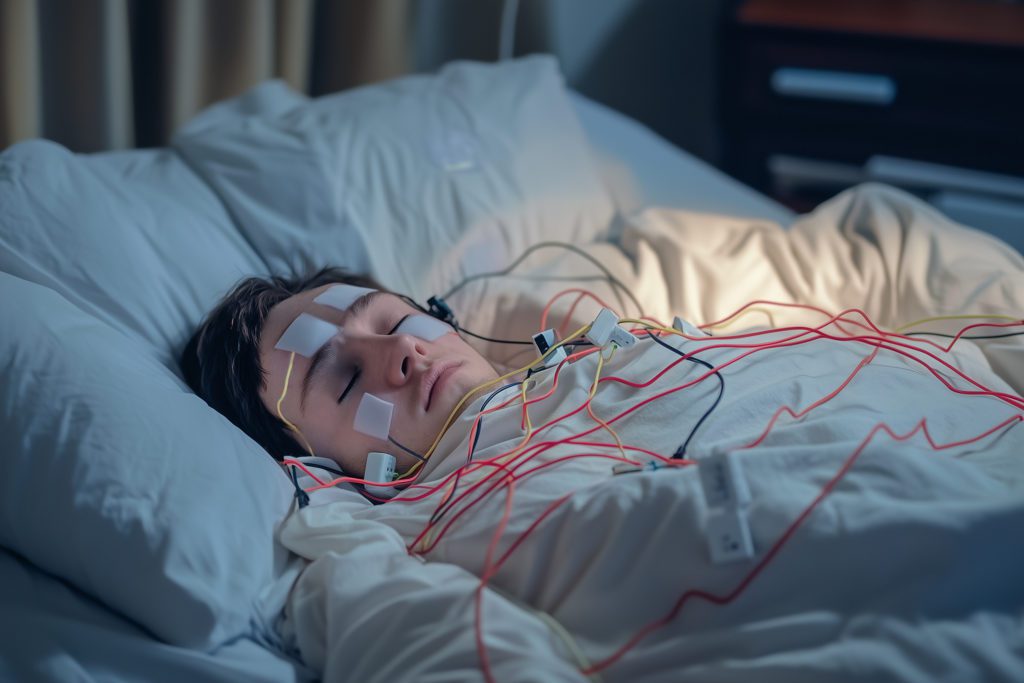
What Are The Most Common Sleep Disorders?
Sleep disorders include a variety of conditions that impact sleep quality and quantity. They can affect someone’s daily function while awake, and may be symptoms of and/or contribute to other physical or mental health issues.

Today, more than 100 specific sleep disorders are recognized by the medical community. But, most of them fall into one of these four main categories:
• Having trouble falling and staying asleep at night
• Having trouble staying awake during the day
• Inability to keep a regular sleep schedule
• Sleep-disruptive behaviors
In this article, we’ll cover five of the most common sleep disorders.
Insomnia
Insomnia causes people to have difficulty sleeping, despite their best efforts to do so. There are three types of insomnia:
Sleep-onset insomnia
Makes it difficult for people to fall asleep even though they feel tired.
Sleep maintenance insomnia
Makes it difficult to stay asleep for the whole night. Specifically, if someone with this type of insomnia wakes for any reason throughout the night, they will have a hard time falling back asleep.
Mixed insomnia
Sufferers exhibit both of the previous types of insomnia and can have a difficult time with both falling asleep and staying asleep.
Since people with insomnia tend to not get enough sleep during the night, they often feel very sleepy during the day and can experience cognitive impairments. Insomnia is classified as chronic when someone experiences symptoms three or more times per week for at least three months.
Statistics show that as many as 33% of adults suffer from insomnia. Fortunately, there are several ways to help alleviate insomnia, including light therapy, cognitive behavior therapy specifically for insomnia (CBT-I), exercise, meditation and other relaxation techniques, medication, and sleep hypnosis.
Hypersomnia
Hypersomnia can cause constant and recurring feelings of extreme tiredness during the day, despite many people with hypersomnia sleeping 10 or more hours per night. They can have difficulty waking up in the morning or after daytime naps, and can sometimes become confused or even aggressive upon waking. Daytime naps don’t tend to relieve sleepiness or improve levels of alertness. Sufferers can also experience anxiety, irritability, restlessness, inability to focus, slow thinking and speech, headache, loss of appetite, and hallucinations.
Hypersomnia can be caused by other medical conditions, such as epilepsy, tumors, encephalitis, obesity, and Parkinson’s disease. Certain mental health conditions can also cause it, including seasonal affective disorder, bipolar disorder, and depression. Medication and alcohol use can lead to hypersomnia.
Narcolepsy, which we’ll cover next, is a type of hypersomnia, although hypersomnia can also be idiopathic—meaning no specific condition or reason can be identified as the cause.
Narcolepsy
Narcolepsy causes people to feel extremely tired during the day, even if they have gotten plenty of sleep the night before. It can cause “sleep attacks” where people spontaneously fall asleep for a few minutes at a time throughout the day. Those with narcolepsy can also experience automatic behaviors while they are technically asleep, disruptions to nighttime sleep, sleep paralysis, and sleep-related hallucinations.
There are two types of narcolepsy: type one (NT1) and type two (NT2). NT1 is associated with cataplexy (a sudden loss of muscle control) and low levels of hypocretin-1 (a chemical that helps control sleep and wakefulness). Those with NT2 do not have cataplexy or low hypocretin-1 levels, although they can eventually develop those symptoms and be reclassified as NT1.
Narcolepsy can significantly impact day-to-day life as everyday tasks such as driving and navigating stairs can be very dangerous when you might fall asleep and lose control of your body at any time. Medicine and behavioral adaptations can help manage symptoms, although there is no cure for narcolepsy and no treatment can completely eliminate all symptoms.
Non-24-Hour Sleep-Wake Disorder
Most people’s circadian rhythms operate on a 24-hour basis, but some people experience shorter or longer than usual sleep-wake cycles. For most of us, environmental cues like the sun rising and setting help our brains and bodies stay synchronized to a 24-hour cycle. However, some people do not have this intrinsic clock.
Non-24-hour sleep-wake disorder (N24SWD) is most prevalent in people who are completely blind, since light-based cues cannot be perceived. In fact, nearly half of those with total blindness have N24SWD. However, sighted people can be affected by this sleep disorder as well, although it can easily be misdiagnosed.
Some treatments can help with N24SWD, although it so far appears to be a lifelong disorder. Medications like melatonin supplements and melatonin receptor agonists are typically taken at a certain time in advance of a person’s desired bedtime in order to help trigger sleep on time. Bright light therapy in the mornings can also be an effective treatment for sighted people or those who are partially blind but can still detect light.
Sleep Apnea
Sleep apnea is a disorder that makes it difficult to breathe while sleeping. It causes people to wake up choking or gasping, and can also cause serious snoring. Since sufferers are often woken by the condition multiple times throughout the night, they can also experience daytime fatigue and sleepiness as well as headaches and cognitive impairment from chronic lack of sleep.
There are two types of sleep apnea:
Obstructive sleep apnea
OSA is caused by a physical obstruction in the upper airway or throat. This can include especially large adenoids or tonsils, fluid buildup, genetic facial structure differences (such as cleft palate), or fat deposits. Obesity is often a cause of obstructive sleep apnea. Additionally, sleeping on your back can allow your tongue to fall to the back of your throat and block your airway.
Central sleep apnea
With CSA, the brain temporarily stops sending signals to the muscles that control breathing, resulting in the cessation of normal breathing. This type of sleep apnea can be caused by problems with the brainstem, which may be caused by stroke, brain infection, or neck injuries. Narcotic painkillers can also cause CSA.
Some people can suffer from both types of sleep apnea at once. Fortunately, both OSA and CSA can often be treated effectively with continuous positive air pressure (CPAP) therapy. However, some find that bi-level positive air pressure (BiPAP) therapy is more effective for CSA specifically.
References
- What are Sleep Disorders?
- Sleep disorders
- Swapna Bhaskar, D. Hemavathy, Shankar Prasad - Prevalence of chronic insomnia in adult patients and its correlation with medical comorbidities
- Richard J. Schwab - Circadian Rhythm Sleep Disorders
- Roneil G. Malkani, MD, MS, Sabra M. Abbott, MD, PhD, Kathryn J. Reid, PhD, and Phyllis C. Zee, MD, PhD - Diagnostic and Treatment Challenges of Sighted Non–24-Hour Sleep-Wake Disorder
- Obstructive sleep apnea - adults
- Central sleep apnea
FAQ
Can your mattress or pillow affect your sleep patterns?
Yes, an uncomfortable mattress or pillow can contribute to poor sleep by causing body pain or improper support. Investing in ergonomic sleep products tailored to your preferences can enhance comfort and sleep duration.
Is napping during the day harmful to your nighttime sleep?
Short naps (20-30 minutes) can boost energy without disrupting nighttime sleep. However, long or late-day naps may interfere with falling asleep at night, especially for those with existing sleep issues.
Why is it harder to sleep well as you get older?
Aging can lead to changes in your sleep architecture, such as lighter sleep and fewer hours of deep sleep. Medical conditions, medications, or lifestyle factors also contribute, making consistent routines even more important.
What are some underrated habits for improving sleep quality?
Small changes like keeping your bedroom slightly cooler, exposing yourself to natural light in the morning, and using white noise or blackout curtains can make a big difference in improving sleep quality over time.
What role does diet and exercise play in managing sleep disorders?
A balanced diet and regular physical activity can promote better sleep by regulating hormones and reducing stress. However, it's important to avoid heavy meals and vigorous exercise close to bedtime.
Are there any natural remedies or alternative therapies effective for sleep disorders?
Natural remedies like melatonin supplements, herbal teas, and practices such as meditation and acupuncture have been found helpful by some individuals. It's advisable to consult with a healthcare provider before starting any alternative therapy.

Written by
Cat Caroll
Articulate Writer and Analytical Editor
Download Pillow
Get help
Press & News
Legal
Connect
X (Twitter)
Affiliates & Partnerships
Company
Copyright © Neybox Digital Ltd.